
Most people do not see the potential danger in the appearance of small epithelial tumors on the body, but papillomas are not only a cosmetic defect. In some cases they can lead to irreversible consequences. Growths appear as a result of infection with HPV - a highly contagious virus that has more than 100 genotypes and some of its types can provoke the development of oncological processes. It is easy to get infected with papillomavirus, so to avoid infection, you need to know how the human papillomavirus is transmitted and what factors contribute to the spread of virions.
All routes of HPV infection
There is a tendency that in families where there is a carrier of the virus, in 50-70% of cases the people around him get infected. The main danger is that the infection, having entered the body, does not appear immediately, so a person may not know about the infection for a long time and continue to be in close contact with relatives.

Important!
The absence of external manifestations of HPV does not guarantee that an infected person is absolutely safe for his close circle.
Infection through family contact
A virus carrier can transmit a pathogenic virion (viral particle) to a healthy person through:
- Common tactile contact, for example, hugs, handshakes. The possibility of contracting HPV increases if there are skin lesions (even small wounds, scrapes or scratches are enough for the infection to penetrate a healthy body);
- Use of personal belongings of a sick person. Viral particles can live for a long time in bedding, towels, underwear, washcloths and other products of daily use;
- During the kiss. HPV DNA is not only found in the epithelium, but is present in all biological fluids of an infected person and therefore can be transmitted through saliva during a kiss.
In addition, you can become infected with HPV when visiting public places such as saunas, swimming pools, fitness centers, where there are large crowds of people, many of whom neglect the basic rules of protection. Therefore, you should use exclusively personal and household hygiene products.
Sexual transmission of the virus
The most common route of transmission of the human papillomavirus is through sexual contact. If one partner, whether a man or a woman, is a carrier of the virus, then it is enough to have sexual intercourse once to be infected with HPV (infection occurs in 95% of cases).
The virus is transmitted through any type of sexual interaction, be it oral, vaginal or anal, while the presence of condylomas in the partner's anogenital area increases the risk of infection up to 100%.
Interestingly, even a condom cannot fully protect against possible infection:
- First, papillomatous rashes can be localized not only on the genitals, but also on the groin and anus. Therefore, by contact with unprotected areas of the body, the virus can be easily transmitted from one partner to another;
- Secondly, the latex from which the condom is made has quite large pores. Viral particles penetrate through them without obstacles.
Infection with dangerous oncogenic types of papillomavirus occurs mainly during sexual contact. If the cancerous type of HPV is transmitted to women, they develop neoplasia, which can develop into cervical cancer.
Despite the fact that oncological pathologies of the genital organs are less common in men, the presence of genital papillomas increases the risk of malignancy. If infection with a cancerous virus occurs during oral sex, the likelihood of developing tonsil cancer increases.
Vertical infection (from mother to child)
Children can be infected with papillomavirus in the womb or immediately at birth (during the passage through the natural birth canal). In addition, if the mother's HPV progresses (is in the active phase), then the risk of infection of the baby increases.

Intrauterine infection is extremely rare, as the placenta is able to protect the embryo from many pathogenic factors, including viral infections. Cases of HPV transmission to a baby during passage through the birth canal of an infected mother are recorded somewhat more often.
At the time of birth, the mucous membranes of the child's larynx and trachea are affected, which then leads to recurrent respiratory papillomatosis (RRP). This is a dangerous pathology that poses a threat to the life of the baby. During 1-2 years, children with RRP develop benign neoplasms of the trachea and larynx, which block the airways and cause suffocation.
In such a situation, only surgical removal of papillomatous growths will help, however, even after destruction, tumors usually reappear. Parents whose children suffer from RRP should carefully monitor the state of their immune system, as decreased immunity increases the risk of relapse.
Some women who are preparing to become mothers worry that the papillomavirus can be inherited from the child, but this is not the case. The routes of infection are described above; the hereditary factor is completely excluded - HPV is a virus that is not genetically transmitted.
The method of autoinoculation of infection
Self-infection (autoinoculation) is a fairly common type of infection. An infected person should understand that any trauma to tumors can cause the formation of additional growths.
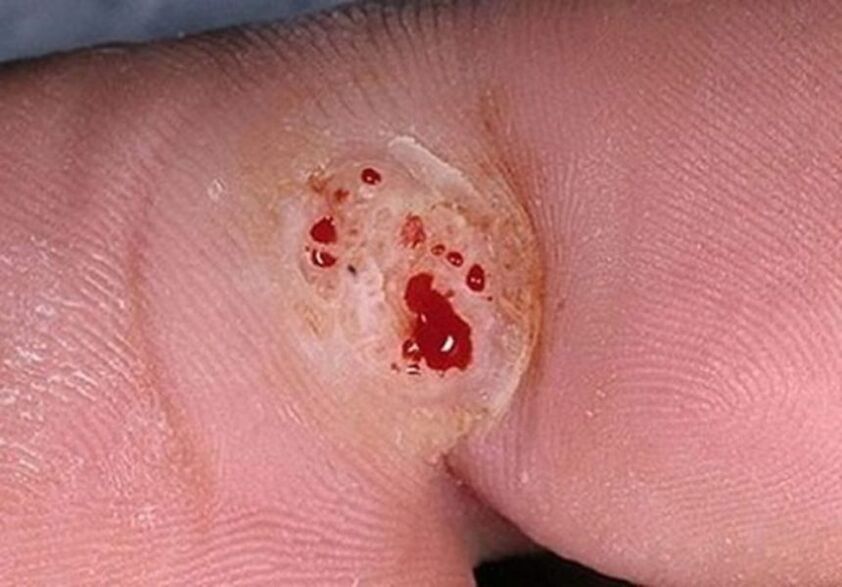
Papillomas located on the face, neck, armpit or groin are often cut with a razor, scratched or torn during hygiene procedures. When the integrity of the growth is broken, blood flows from it and flows into adjacent healthy areas of the body. Since viral particles are present in all biological fluids of the patient, blood entering the clean epithelium causes the spread of infection and the formation of numerous papillomatous rashes.
In addition, when you scratch growths with nails, particles of pathogenic epithelium remain under the plates, which also often contributes to self-infection. For example, after a person has scratched a papilloma with his nails and he suddenly decides to scratch his ear or nose, then if there is even the slightest damage to the epithelium, the virus will definitely "settle" in it and then appear. as characteristic growth.
After entering the body, the activation of HPV is not immediately observed, the virus requires certain conditions for full functioning.
When and what causes HPV activation
How quickly and actively the papillomavirus begins to behave after infection is determined by the immune status of the infected person. HPV belongs to the group of immune-dependent viruses, so its activation occurs during a decrease in immune defense.
The body of a healthy person, even after infection, is able to produce a sufficient amount of antibodies to completely resist viral attacks. In such people, the disease continues latently (in a dormant state), so there are no epithelial tumors in the body.
When the immune system is weakened, it produces a significantly smaller amount of antibodies that cannot independently suppress the virus, and then HPV becomes active with the formation of a papillomatous rash. The following unfavorable factors can provoke the transition of the papillomavirus to the active phase:
- any recently suffered pathology of an infectious nature;
- long-term use of oral contraceptives;
- uncontrolled use of cytostatic drugs (suppression of the immune system);
- dysfunction in the endocrine system;
- pathological condition of the gastrointestinal tract, in particular intestinal dysbiosis;
- psycho-emotional disorders associated with frequent stress, irritability, fatigue;
- helminth infections;
- frequent inflammatory skin diseases;
- the presence of bad habits (smoking, drinking alcohol, drugs).
Important!
Any factor that reduces the effectiveness of the human immune system can cause the activation of HPV.
The formation of the first growths is a reason to consult a doctor. There is no need for self-medication, as in some cases inadequate therapy for papillomas leads to the development of cancerous tumors.
Treatment of papillomavirus
Since drugs that can cure papillomavirus have not yet been invented, it is impossible to completely remove it from the body for a person after 30 years. Cases of HPV elimination are recorded only among young people under 25 years of age.
Treatment of papillomatosis is carried out in three directions:
- suppression of viral activity (returning it to a latent state) by taking antiviral drugs;
- increasing the patient's immune status through the use of interferon drugs;
- destruction of pathological neoplasms using minimally invasive hardware techniques;
- cytostatic drugs are prescribed when there is a high probability of malignancy of papillomas (they disrupt the process of division of atypical cells).
Antiviral medications prescribed by a doctor can be for oral, topical, injection or rectal use:

- Tablets (oral use);
- Gel, ointment (external use);
- Injections (shots);
- Suppositories (rectal suppositories).
Immunomodulating drugs can also be prescribed in different forms, most often these are tablets and gels for the external treatment of tumors.
Cytostatics are prescribed if, after the diagnosis, it is found that papillomatous rashes are provoked by a highly oncogenic type of HPV.
The destructive techniques that are most often used to remove pathological tumors are:
- Electrocoagulation- cauterization of growths with electric current. The procedure is painful and leaves visible marks;
- Cryotherapy– the papilloma freezes under the influence of liquid nitrogen, leaving no trace behind, but the procedure is recommended for the removal of small superficial tumors;
- Laser destruction– suitable for removing superficial and deep papillomas, a good cosmetic effect makes it possible to use on open parts of the body;
- Radio wave technique- The growths are removed without contact, with a short recovery period, there are no traces or scars after the intervention.
After completing the course of treatment, do not forget about preventive medical examinations. It is necessary to periodically (preferably every year) be tested for HPV, and also carefully monitor the state of the immune system.




















